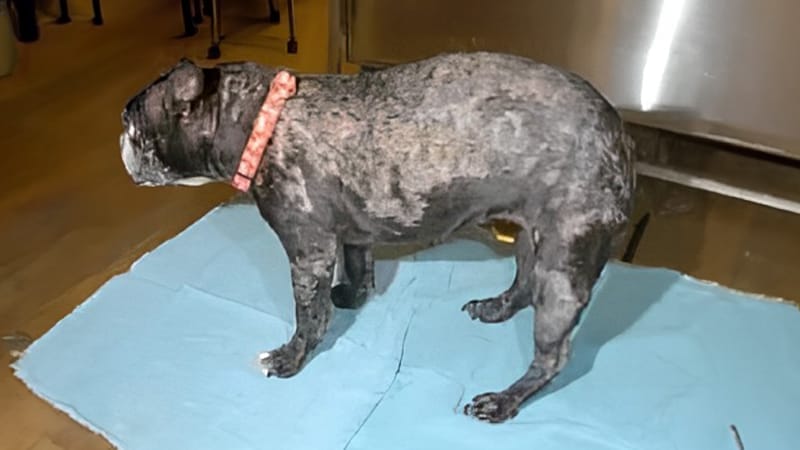
On initial presentation, “Puppy” was an otherwise healthy 5-year-old, spayed Boston Terrier with a progressive crusting dermatitis of several months’ duration. She was also moderately “itchy” where there were lesions. “Puppy” was treated with antibiotics by her primary care veterinarian for superficial bacterial folliculitis without any improvement in the lesion severity.
Antihistamines were prescribed for itching but did not alleviate the issue. Puppy was referred to a veterinary dermatologist. Upon examination, there were widespread 1 cm round lesions that coalesced to form thick, yellow-colored crusts. Lesions were located the ear pinnae, trunk, abdomen, chest, limbs, and face. Several causes of this crusting dermatitis were considered.
These differentials included superficial bacterial folliculitis (bacterial skin infection) secondary to a primary allergy (which would cause itch), demodex mites, dermatophytosis (ringworm), sarcoptic mange (because she was so itchy and the ear margins were involved), and autoimmune diseases.
Diagnostic Testing
Initial diagnostic tests that were performed included skin surface cytology to look for bacteria, deep and superficial skin scrapings to look for demodex mites and sarcoptic mange mites, and a dermatophyte culture to evaluate for ringworm.
There were no bacteria or mites found and the dermatophyte culture was negative. However, on skin surface cytology, there were numerous eosinophils, neutrophils, and acantholytic cells. Acantholytic cells are a type of skin cell that is found in certain autoimmune skin diseases.
The presence of this cell type and the lack of other evidence to support an infectious or parasitic cause of the lesions, prompted us to perform skin punch biopsies. These skin samples were submitted for review by a dermatohistopathologist. A tissue sample for bacterial culture and susceptibility testing was also submitted to a microbiologist to further document that the lesions were not being caused by bacteria.
The culture did not grow bacteria. The interpretation of the skin biopsies confirmed the diagnosis of pemphigus foliaceus. This form of pemphigus is the most common autoimmune skin disease identified in the dog.
Treatment
The initial treatment for her disease was prednisone at doses to induce immunosuppression and halt the disease process. Azathioprine was later added for additional control. Over several months, her dosages of prednisone were carefully tapered, and the Azathioprine was continued every other day. Antihistamines and soothing bathing therapy was used to minimize itch.
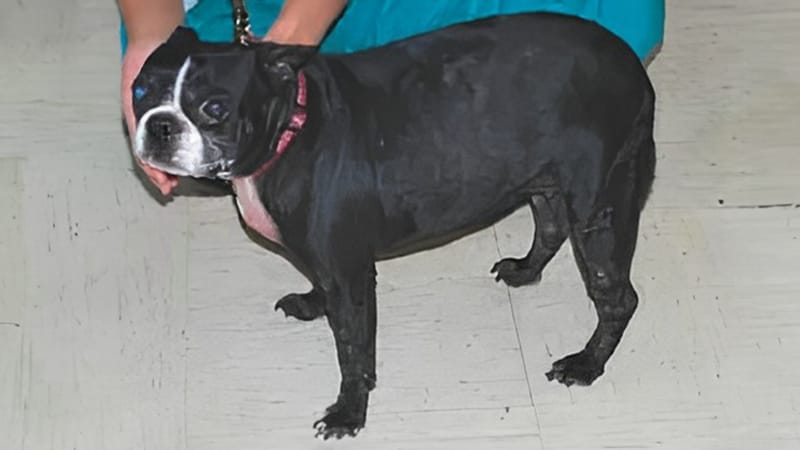
“Puppy’s” pemphigus remained in remission, and she did well for many years under the care of veterinary dermatologist and her primary veterinarian. The veterinary dermatologists who cared for her adjusted medications and monitored her laboratory work several times per year to ensure she was tolerating the immunosuppressive medications.
Working with a Veterinary Dermatologist
This case summary demonstrates how veterinary dermatologists approach crusting dermatitis. After history taking and complete examination, the veterinary dermatologist will form a list of potential causes of the lesions. This list then dictates what tests to perform and typically involve basic in-hospital procedures. Once the gathered information is assessed, a confirmatory test may be performed.
In cases such as pemphigus foliaceus, it is important to confirm the diagnosis prior to treatment. This case also demonstrates how prednisone is used in veterinary dermatology. While our preference is often to minimize usage of corticosteroids such as prednisone, some diseases require it. Pets can do very well and live a normal life-span while on prednisone if they are carefully monitored by their veterinary dermatologist.