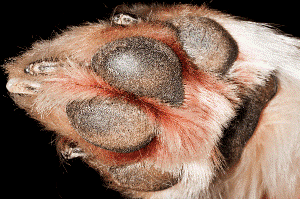
Nail diseases are very interesting to diagnose and treat as a veterinary dermatologist. Infections (bacterial paronychia, onychomycosis), immune mediated diseases (SLE, Pemphigus vulgaris, bullous pemphigoid), trauma, tumors (melanoma, squamous cell carcinoma, keratoacanthoma), inflammatory (vasculitis), metabolic (hepatocutaneous syndrome), and other conditions (nail bed inclusion cysts) may affect the nails and/or nail bed epithelium.
Signs of Symmetric Lupoid Onychodystrophy
In dogs, there is an interesting nail disease called symmetric lupoid onychodystrophy/onychitis (SLO) that should be considered when a dog is presented with the following clinical signs: onychalgia (pain), oncholysis (splitting of nail), or onychomadesis (nails falling off). What was previously considered a pathognomonic histopathologic pattern noted in nail biopsy specimens from affected dogs is now known to occur in other diseases affecting the nail (e.g. leishmaniasis). So, some consider SLO a reaction pattern rather than a specific disease. Additionally, in older reports on this condition, previously described features are now known to occur in other diseases as well.
SLO is an uncommon disease of the claw in young adult to middle aged dogs. The nail problem originates in the claw bed and the cause is not yet known. SLO is recognized most often in the large breed dogs, but it has been reported in the following breeds: German Shepherd, Rottweiler, Labrador Retriever, Gordon Setter, Cavalier King Charles Spaniel, Schipperke, Welsh Corgi, West Highland White Terrier, Bearded Collie, Miniature and Giant Schnauzers, Akita, Greyhound, and German Short Hair Pointer.
Typically, the first observation is licking of the nails (due to onychalgia) or lameness. Claws elevate from the nail bed. Loss of the nail, onychomadesis, will occur. Over a relatively short period of time all nails on all paws are variably affected. Claws regrow, but they will be misshapen, dry, brittle, and crumbly. Bleeding (hemorrhage) beneath a retained nail may be recognized. Secondary bacterial infections may be seen as well as regional lymphadenopathy. Typically no other medical symptoms are identified.
Symmetric Lupoid Onychodystrophy Diagnosis
An initial diagnostic test that is commonly performed by the veterinarian is cytology to look for infection. If bacterial or yeast infections are identified, they are treated first. If symptoms persist, biopsies may be performed, as histopathology is used to confirm a clinical diagnosis of SLO. Bacterial and fungal cultures may also recommended. Optimal biopsy specimens are obtained by a P3 digit amputation (the distal aspect of a phalanx). The dewclaw is the preferred site. Sloughed claws do not usually contain the claw bed, the location needed for the diagnosis. For the cultures, a sloughed claw (newly) may be used. With biopsy, tissues are routinely processed for histologic evaluation and stained with H & E stain. Decalcification may be performed. There is an inflammatory reaction with a notable lymphohistiocytic (both B and T lymphocytes) and mild plasmacytic interface dermatitis with basal cell degeneration, apoptosis, and pigmentary incontinence of the claw bed epithelium. Lupoid onychitis or SLO is the etiologic diagnosis.
Symmetric Lupoid Onychodystrophy Treatment
Treatment is usually very safe, but takes several months to appreciate a response to therapy due to the slow growth of a claw in the dog. Expect treatment to be life-long. If treatment is discontinued, the dog will have recurrence. Tetracycline or doxycycline with niacinamide is one option. Supplemental omega 3 (and omega 6) fatty acids are usually a cornerstone of treatment. Biotin may be given orally with meals for nail strengthening properties. Pentoxifylline has been used adjunctively, with variable results. More aggressive treatments with glucocorticoids, azathioprine, cyclosporine or onychectomy are rarely prescribed. Diligent claw treatment and paw hygiene recommended. Diets enhanced with fatty acids are sometimes utilized when pets are reluctant to take oral fatty acid supplementation or need additional sources.
SLO is a very clinical diagnosis supported by confirmatory tests. If you are a veterinarian with a possible case, consider the diagnostic work up and treatment.